Rise of major depressive disorder: The burden of modern society
The ongoing pandemic has reminded us that the health for all goal cannot be achieved without paying attention to people’s mental health. Despite increasing emphasis on improving mental healthcare, there is an urgent need for greater specificity regarding policies and treatments tailored to mental illnesses.
KPMG, Johnson & Johnson, as well as many healthcare practitioners across Southeast Asia, have undertaken extensive field research over the past year on major depressive disorder (MDD). The results of the research will be shared with policy leaders to foster public-private partnerships to shape the future of MDD care pathways. The report highlights challenges and lessons, and concludes with a recommended path ahead, together with bespoke country-level considerations.
Matthias Skillecorn, managing director of Johnson & Johnson Vietnam, said, “Mental health requires more attention than ever before, especially as the pandemic has exacerbated the mental distress faced by many people. The study outlines the mental health picture in Southeast Asia and in Vietnam, providing policymakers and healthcare practitioners with specific policy recommendations to treat and care MDD patients and to reduce the burden this disease puts on families and the healthcare system. It is important that ‘no one is left behind’ to actualise the vision of ‘health for all’.”
According to the Disease Indicators of Vietnam in the research, the number of people suffering from mental illness and neurodevelopmental disorders was 9.6 million. MDD accounted for 1.2 per cent; the percentage of patients with mental disorders with suicidal ideation (MDSI) among that was 21 per cent in 2021 and the suicide rate was 7,4 per 100.000 people in 2017.
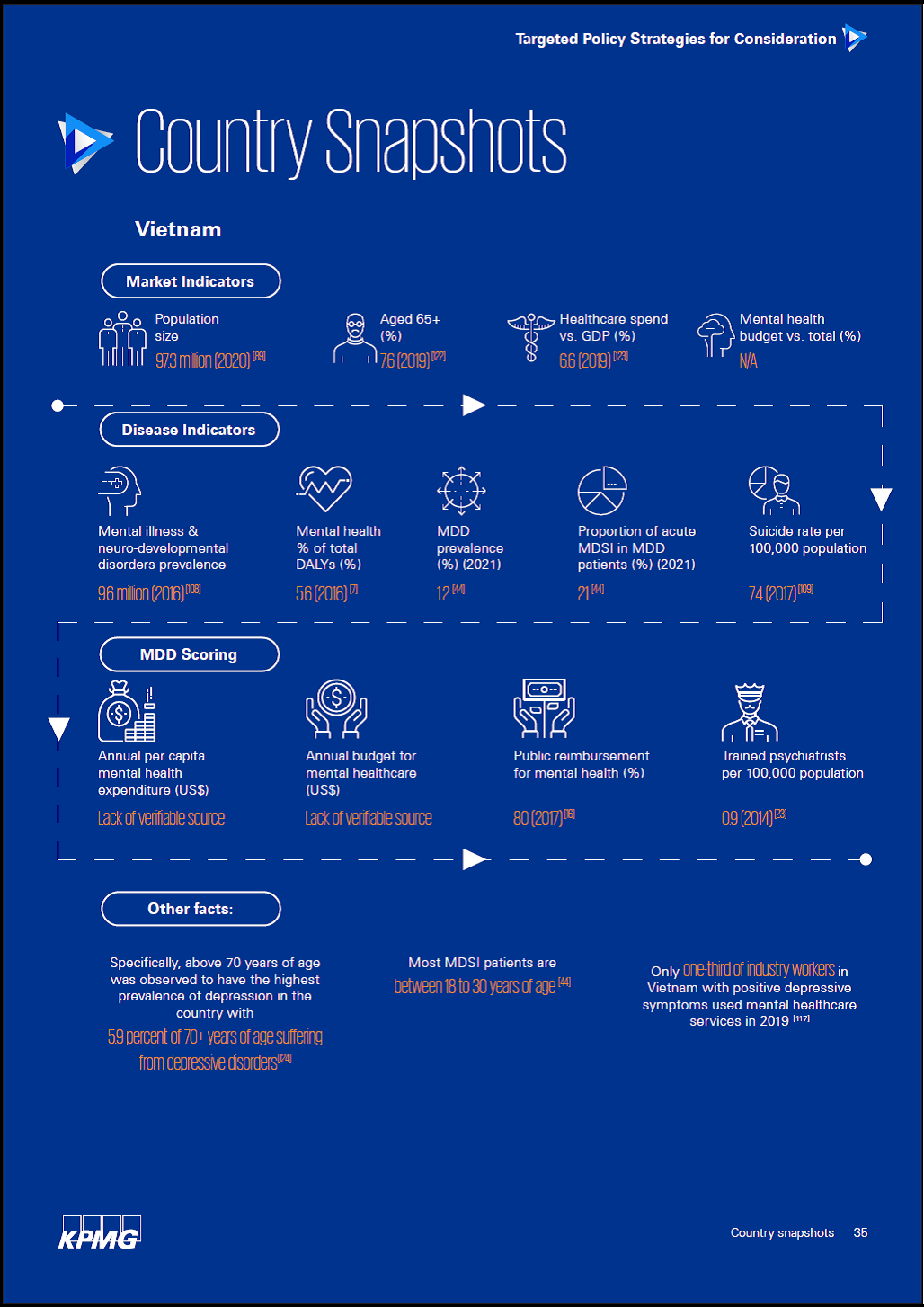 |
In 2019, up to 5.9 per cent of people over 70 years old in Vietnam suffered from depressive disorders, while most patients with MDSIare between 18-30 years old. However, only one-third of the people with symptoms of depression accessed mental health services in 2019, according to the results of research.
Vietnam is currently implementing several national mental health policies, but budgetary allocations for the cause remain limited. There is also a lack of trained psychiatrists, with less than one (0.9) professional available for 100,000 inhabitants, much lower than the recommendation of 10 by the World Health Organization.
Vietnam has made impressive progress in improving the capacity to treat mental illnesses over the past decade and added depression to its National Health Target Program with its Community-Based Mental Health Care (CMHC) Programme since 2001.
CMHC includes screening, referral, treatment, management, and monitoring among primary health centres, district and provincial hospitals, and third-class medical facilities. However, only 2 per cent of the programme’s participants received treatment for depression.
This shows that frontline healthcare and higher-level hospitals are not closely linked. Therefore, there is a need for more comprehensive mental healthcare networks, improved resources, mental health infrastructure, and increased information dissemination.
What the stars mean:
★ Poor ★ ★ Promising ★★★ Good ★★★★ Very good ★★★★★ Exceptional
 Tag:
Tag:
Themes: Healthcare Platform
Related Contents
Latest News
More News
- Ministry of Health issues list of free regular health check-ups (May 13, 2026 | 18:34)
- Health-related community campaign launched in Hanoi (May 13, 2026 | 18:29)
- Health Ministry to implement free health check-ups (May 08, 2026 | 09:00)
- Hanoi mulls time-based petrol motorbike ban on 11 streets (April 23, 2026 | 17:16)
- Government launches regular health checks alongside food safety crackdown (April 22, 2026 | 10:18)
- Vietnam recognised among top performers in World Bank human capital index (April 20, 2026 | 20:32)
- VCCI refutes US concerns over overcapacity and forced labour in Vietnam (April 17, 2026 | 17:22)
- Vietnamese among Asia’s most optimistic spenders (April 14, 2026 | 16:49)
- MoH urges hospitals to accelerate electronic medical records (April 13, 2026 | 14:19)
- Hanoi considers easing pickup truck restrictions to support businesses (April 02, 2026 | 15:52)





























 Mobile Version
Mobile Version