Hospitals bemoan autonomy trial flop
The Vietnam National Cancer Hospital (K Hospital) is planning to submit a proposal to the Ministry of Health (MoH), seeking to withdraw from the list of central hospitals with comprehensive autonomy in October when its trial period comes to an end.
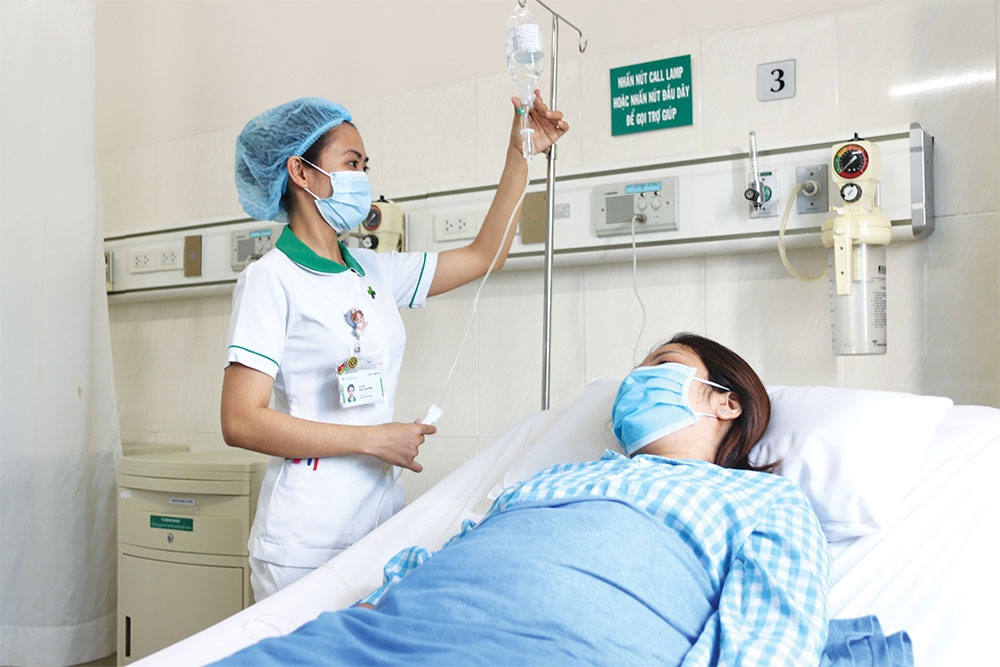 |
| Hospitals may need further investment in order to successfully reach full autonomy, Le Toan |
Hospital director Le Van Quang said, “We faced many challenges since piloting autonomy as we could not make our own decisions about hospital fees. The hospital has to follow the common regulated price frame. We also have no right to decide about human resources, but instead must report to the MoH.”
K Hospital will follow Bach Mai Hospital, which proposed a halt to hospital autonomy at a meeting with acting Minister of Health Dao Hong Lan on August 18.
Dr. Duong Duc Hung, chairman of the Hospital Management Council, blamed a lack of a comprehensive legal framework for the situation. “Since 2020, Bach Mai has been assigned to do comprehensive autonomy. However, it has never had sufficient conditions for autonomy, including the right to self-control its organisation, prices, and other matters. This means that the hospital only carries out autonomy on paper.”
Bach Mai director Dao Xuan Co added, “There should not be any comprehensive autonomy at central hospitals in this period of time, but instead autonomy of regular spending. We need support from the government and the MoH during this.”
Bach Mai Hospital and K Hospital are among four state-owned central hospitals piloting comprehensive autonomy, together with Viet Duc and Cho Ray since 2020. Like others, Bach Mai suffered a serious pandemic impact as revenues fell by around $174 million compared to 2019.
Under Resolution No.33/NQ-CP issued in 2019 approving the pilot of comprehensive autonomy, hospitals are able to make decisions about the prices of medical and treatment services in line with the price frame issued by the MoH. However, according to the four hospitals, the medical pricing framework is now outdated. Meanwhile, there is no ceiling price for customised medical services, making it difficult to decide on reasonable prices.
Nguyen Thi Hong Nhung from Bach Mai Hospital’s Financial Accounting Division said, “A hospital cannot do comprehensive autonomy if the medical price framework is comprised of just four out of seven price components. In fact, there are some medical services whose prices are comprised of just one price component, especially surgery services.”
Moreover, the autonomy model at hospitals has proved problematic as the roles of the management board and the board of directors are overlapping, making it difficult to define who truly has the final say on matters.
With the trial difficulties, operating central hospitals in the model of private-run ones without state funding could be a diminished prospect.
According to experts, hospital autonomy should enable the healthcare industry to ensure financial resources for development. However, the lack of support at the same time as hospitals had state funding cut and suffered hardships from the pandemic played against the goals. To enable hospitals to carry out part-autonomy, regular spending autonomy, or comprehensive autonomy, it is necessary to have a more concrete legal framework.
Nguyen Anh Tri, former director of the National Institute of Hematology and Blood Transfusion, said, “The state asks hospitals to do autonomy, but did not craft a mechanism to allow them to self-control finance, medical service prices, and manpower. To enable the success of hospital autonomy, a number of regulations must be amended first.”
Dr. Nguyen Duc Kien, head of the Economic Advisory Group to the Prime Minister, blamed the trial failures on the pandemic, lack of experience in implementation, and insufficient preparations and investment. The MoH should therefore encourage the hospitals to continue the autonomy process.
“Each hospital has its own peculiarities. Therefore, to enable autonomy, there should not be the same model for all. There should be specific decisions or decrees about the trial for each hospital. From now to the end of 2022, the MoH should submit to the prime minister for issuance four specific decisions about the trial of autonomy for the four hospitals already involved.”
In the long term, the MoH should study and submit by 2025 to the prime minister a draft resolution on renovating the organisation of the health sector’s apparatus to ensure innovation in health work in the context of industrialisation and increasingly global economic integration, according to Kien.
 | Accelerating the vital digital transformation of hospitals In recent years the healthcare sector has made breakthroughs in IT application, and approaching digital technologies like the Internet of Things, AI, VR, cloud computing, big data, and more. All hospitals nationwide deploy hospital management information systems, while interconnectivity with the healthcare insurance payment verification system has reached 99.5 per cent. Around 20 health facilities deploy electronic medical records in substitution for paper ones, and 23 hospitals deploy picture archiving and communication systems. |
 | Drugs shortfall requiring clean-up via authorisations Vietnam’s health sector is still challenged by a shortfall of drugs and medical devices in the post-pandemic landscape, urging a strong legal reshuffle ahead to increase business facilitation and market certainty. |
 | Post-pandemic staff headaches continuing for local hospitals While local state-owned hospitals are facing a headache with health staffing, foreign-invested groups are performing well with qualified manpower. |
What the stars mean:
★ Poor ★ ★ Promising ★★★ Good ★★★★ Very good ★★★★★ Exceptional
Themes: Healthcare Platform
Related Contents
Latest News
More News
- Shopee fined for misleading promotion information (May 20, 2026 | 11:02)
- Coffee sector shifts to deep processing as export markets demand more (May 20, 2026 | 10:56)
- Hai An plans $75 million bond issuance to expand container fleet (May 20, 2026 | 10:14)
- Searefico broadens industrial and renewable energy footprint (May 20, 2026 | 09:52)
- Vietnam enters Top 50 global startup ecosystems (May 20, 2026 | 09:00)
- VinaSugar Holdings enters voluntary liquidation in BVI (May 19, 2026 | 20:00)
- PC1 Group says business stable as it cooperates with authorities (May 18, 2026 | 14:00)
- How should Vietnam approach renewed oil market volatility? (May 18, 2026 | 09:00)
- Vietnam maintains stable AI outlook in 2026 survey (May 18, 2026 | 09:00)
- Robotic surgery at FV Hospital removes stage 3A lung tumour (May 18, 2026 | 09:00)

 Tag:
Tag:




















 Mobile Version
Mobile Version