Harnessing AI for healthcare revolution
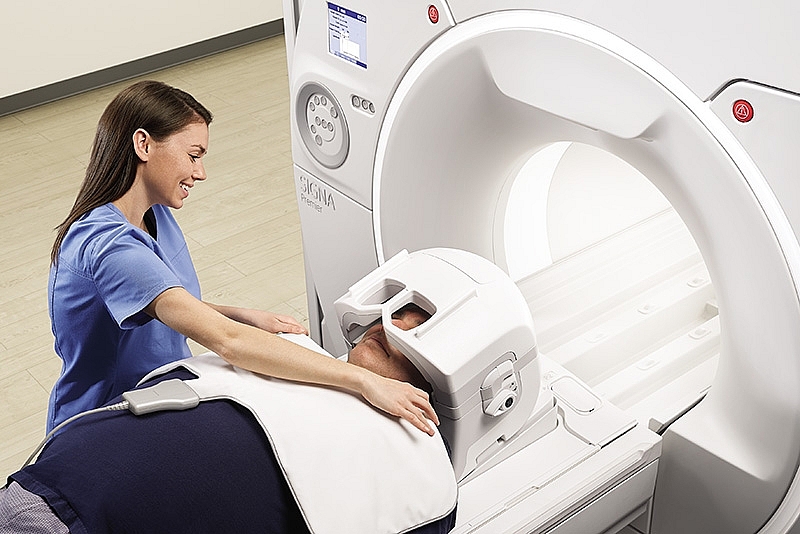 |
| GE’s AI-driven solutions offer plentiful advantages before, during, and after medical procedures |
In the past, patients were diagnosed and treated in the same way – without regard to each individual being fundamentally unique. However, the healthcare sector is now departing from evidence-based medicine to precision medicine to tailor diagnostics and therapy to the circumstances and personal needs of each and every patient.
Nowadays, data is surrounding people and AI can help us take in and use all this data. In fact, people are surrounded by AI in every waking moment of every day. When people look something up on Google, they become part of the deep learning algorithm. Clicking on any of the suggested links serves as feedback for Google. The more people search for a term and the more they click on a particular link, the more it will come up in subsequent searches. And this is just one example of deep learning and AI that are permeating even our most mundane daily activities.
AI for image diagnostics
A report from Accenture highlighted the value of AI in healthcare, concluding that it is worth its hefty cost. Accordingly, AI can save $150 billion annually on healthcare spending in the United States.
In a talk with VIR about the potential of AI in healthcare, Prof Dr Mathias Goyen, chief medical officer in Europe at GE Healthcare, the leading global medical technology and life sciences company, said that AI can help at the individual, department, and enterprise levels.
At the individual level, AI can be implemented in machines, devices, as well as CT, MRI, and ultrasound systems. The AI can be used before, during, or after the scan. Instead of manually processing slices, GE Healthcare makes a smart scanner which will free up technicians to spend more time explaining findings to patients and talking with doctors.
“We have built-in AI capabilities on our MRI systems that can automatically detect where the brain is, and it automatically suggests the right sequence and automatically suggests the optimal cross-sectional images, or slices, of the brain to acquire,” Goyen explained, taking only one example of how AI can be used before scanning.
Another possibility is to use AI during the scan. In ultrasound, the radiologist usually starts the scan, finds the region of interest, and then they press a button. The algorithm built into the machine can differentiate, in this case, between arteries and veins, based on different flow profiles. This enables people with less experience to read an ultrasound scan, which will be a great boon in rural areas where there is no doctor to do the scan, only a nurse.
After the image is taken, AI can support the diagnosis. One condition that doctors in the hospital fear is pneumothorax, better known as a collapsed lung. It can be deadly unless detected on time. In fact, it may take several hours before the radiologist actually views the image.
GE Healthcare has also developed a portable mobile X-ray system that has built-in AI capability to alert technicians when the algorithm detects a case of collapsed lung. The system was built by analysing and comparing the images to a large database of other images from patients with collapsed lungs, and has a 95 per cent likelihood of correct diagnosis.
“It is immaterial whether the radiologist is better than the AI or vice versa. It is about increasing the chances of timely diagnosis,” Prof Goyen emphasised.
 |
Smart hospitals
In addition to machines, AI can be used to streamline the workflow in an entire radiology department. AI and deep learning can, first of all, streamline MRI protocols for efficiency without sacrificing image quality, which drives down examination time by 16 per cent.
In addition, imaging insights help optimise the radiology workflow and electronic patient records. As the examination time is reduced, doctors can scan more patients in the same amount of time, and productivity goes up. With the help of AI, waiting times can be reduced from six to two weeks. “A nice side effect is that the revenue increases at the end of the year because the more patients they scan, the more money the hospital earns,” said Prof Goyen.
Globally, GE Healthcare applies AI for predictive analytics to better manage the patient flow throughout the hospital. Two bottlenecks are the ER and the ICU department, the room with a lot of screens showing a lot of data such as the number of vacant or occupied beds, the number of patients, and wait time.
GE Healthcare has already developed 11 command centres across the world, which streamline workflow to increase the number of patients coming to the ICU every day. “In Toronto, by using the command centre, they were able to increase daily visits by 8 per cent and, importantly, they can virtually add an equivalent of 23 beds. They do not physically add those beds but the beds are used at a higher efficiency because you have full transparency of where the free beds in the hospital are, while manual calling does not give you an accurate reading,” said Prof Goyen.
This is not fiction, most of these applications are already reality, and the pace of development is also helping to reduce the cost of these technologies, gradually making them more feasible and providing superior healthcare to people across the globe.
What the stars mean:
★ Poor ★ ★ Promising ★★★ Good ★★★★ Very good ★★★★★ Exceptional
 Tag:
Tag:
Related Contents
Latest News
More News
- Addressing Vietnam's energy challenges with aeroderivative gas turbines (February 28, 2023 | 09:33)
- How to sprint ahead in 2023’s worldwide energy priorities (February 08, 2023 | 13:55)
- Boosting Vietnam's grid stability through gas turbine technology (November 22, 2022 | 20:02)
- Healthcare trio collaborates to provide thousands of free breast scans (October 27, 2022 | 17:19)
- GE Healthcare's vision for AI-backed radiology (September 29, 2022 | 11:53)
- GE brand trio to shape the future of key industries (July 19, 2022 | 15:35)
- GE unveiling brand names and defining future (July 19, 2022 | 15:16)
- GE: the shortest route towards sustainability (July 18, 2022 | 08:00)
- Be proactive in an uncertain world (May 20, 2022 | 11:40)
- GE secures first 9HA combined cycle power plant order in Vietnam (May 16, 2022 | 17:06)






















 Mobile Version
Mobile Version